Yesterday, Tammy Tolleson Knee (the new director of the Phyllis J. Washington Center for the Advancement of Positive Education) and I arrived in Kalispell, Montana for a 2+ day retreat with staff from the Nate Chute Foundation (NCF). Their mission: The Nate Chute Foundation supports, educates and empowers our community to promote mental wellness and reduce suicide. You can learn more about NCF’s fabulous work and staff right here: https://www.natechutefoundation.org/
Our retreat is top secret, but I’ll share it here anyway because I don’t like secrets.
Having grown weary with traditional, pathology-oriented approaches to “suicide prevention” we’re working together to create a new curriculum tentatively titled “Strengths-Based Suicide Education for Concerned Adults.” Our plan is to use this new curriculum to replace all the unhelpful and sometimes traumatizing approaches to suicide prevention.
Yes, we have big goals.
Today we’re breaking away from our retreat for a short presentation/consult with Immanuel Living of Kalispell.
In preparation for this short conversation, I pulled out an old slide about a thing called Stress Inoculation Training (thanks Don Meichenbaum!).
The point of SIT is to prepare for stressors or provocations in life that adversely affect us. For example, let’s say that you find ___________ stressful. (You can put anything in the blank. It could be exercise, talking with your boss, going to church, not going to church, speaking in public meetings, etc.). Then you create your own personalized stress inoculation plan.
Meichenbaum’s therapy approach is designed to prep or inoculate us from our usual and predictable stressors. He described three steps: (1) preparation for provocation, (2) coping with the provocative situation, and (3) reflection and self-reinforcement. Here’s a visual, with our stressors and responses organized into 7 dimensions:
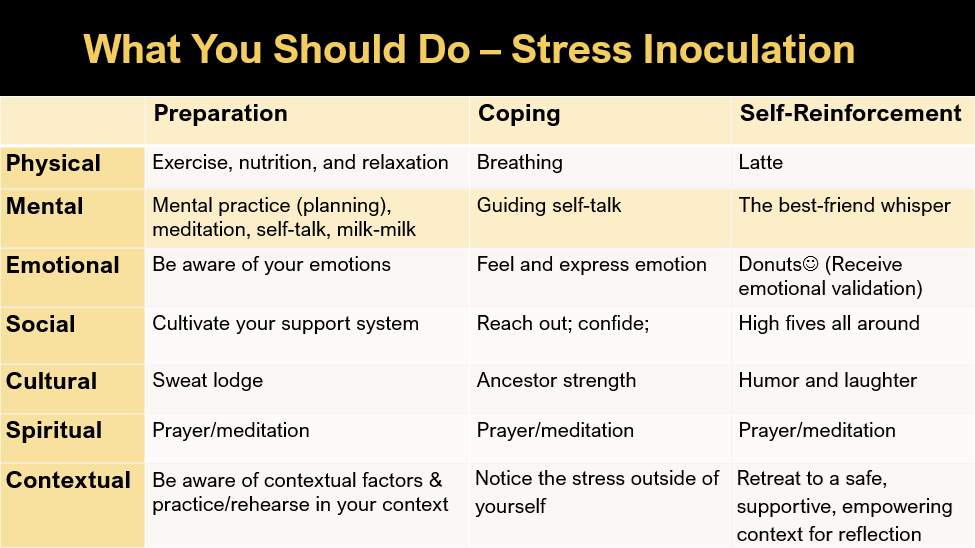
If we all had rational brains and lived in a rational world, SIT would work perfectly for everyone. But like everything, it doesn’t always work. During today’s talk, I’m revealing the secrets of why our best laid plans often fail. Newsflash: it has to do with our quirky brains, which, although amazing, also automatically and regularly take us down into negative thinking rabbit holes.
TBH, IMHO, dipping into a negative thinking rabbit hole every once in a while can be fun, but if your intention was to avoid negative thinking rabbit holes, they’re considerably less fun.
Unfortunately, due to time limits and the need for mystery in marketing, this blog is ending without me sharing the five secrets of why our pesky brains often derail us from our positive intentions. Sorry about that. They’re in the pdf of the ppts linked below, and although you can find them there, it’s much more fun for us to talk about these in person . . . so I hope to see you at a presentation in the future.